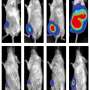
Low-dose chemotherapy protocol relies on normalization of tumor blood supply
The effects of a promising new approach to chemotherapy that involves frequent administration of dosage levels much lower than traditionally used appears to rely on the "normalization" of blood vessels within and around a tumor. In their report receiving online publication in PNAS, a team led by a Massachusetts General Hospital (MGH) investigator describes how their mathematical model, based on data from previous studies, reveals the mechanisms by which what is called metronomic chemotherapy improves both the direct killing of cancer cells by chemotherapy drugs and activation of the immune system again the tumor.
"Standard chemotherapy protocols are based on the administration of the maximum tolerated dose - one that does not produce intolerable toxicities - with drug-free breaks from two to three weeks to allow patients to recover from the side effects," says Rakesh K. Jain, PhD, director of the Steele Laboratories of Tumor Biology in the MGH Radiation Oncology Department, co-corresponding author of the report. "Metronomic chemotherapy has been proposed as an alternative based on frequent, low doses and few drug-free breaks. While this strategy has shown promise in animal models and clinical trials, the underlying mechanisms have not been fully understood."
Several previous studies have suggested a number of potential mechanisms of action for metronomic chemotherapy. While considerable evidence indicated that it primarily functioned as an antiangiogenic therapy, removing blood vessels supplying a tumor, other studies found that it switched the tumor microenvironment from suppressing to enhancing antitumor immune system activity. It also was possible that the treatment's effects on tumor-associated blood vessels could improve delivery of both chemotherapy drugs and oxygen to tumor cells.
No previously developed mathematical model of metronomic chemotherapy accounted for the complex interactions among cancer cells, immune cells and tumor blood vessels. To resolve the diverse results of earlier studies, the research team, including investigators from the University of Cyprus and Bucknell University, developed a model based on all published data on the protocol's effects. Their model accounts for the treatment responses of three different types of cancer cells—stem-like cancer cells, which are more resistant to chemotherapy; non-stem cancer cells and cells that are beginning to acquire stem-like characteristics in response to chemotherapy—of immune cells and of tumor blood vessels along with their interactions.
Preliminary analysis of the model by simulating the growth of a mouse tumor over 30 days, with weekly chemotherapy treatment, revealed that alleviating the abnormal structure and function of tumor blood vessels was a prerequisite for all the beneficial effects of metronomic chemotherapy. Not only would improvements to the vascular network produced by increased expression of the angiogenesis inhibitor thrombospondin-1 increase drug delivery to all types of cancer cells, but increased oxygen in the tumor environment would stimulate immune cell activity and reduce the proliferation of stem-like cancer cells.
The team then used the model to compare the predicted effect of five different approaches - a weekly maximum tolerable dose protocol and four metronomic chemotherapy dosage/frequency protocols - all of which delivered the same total dose over a 30-day period. The comparison revealed that determining the best dosage and schedule would depend on how long tumor cells took to recover from a particular dose of chemotherapy. Specifically, the interval between treatments could be no more than 40 percent of a tumor's recovery time in order to prevent relapse. Use of the model to analyze data from three published studies of metronomic chemotherapy in mouse models predicted results that closely matched the actual reported results.
"This study is an example of how a systems biology approach can yield insights that would be difficult to obtain from a focus on the individual aspects of a complex system," says Jain, who is the Cook Professor of Radiation Oncology (Tumor Biology) at Harvard Medical School. "Only by assembling all the known pieces into a comprehensive model are we able to see how the system as a whole emerges from the complex feedback loops within the system."
He continues, "Our new insights into the effects of metronomic therapy provide some initial guidelines for its optimal use. The most important conclusion is that better treatment outcome depends on the improvement of a tumor's blood supply through vascular normalization - something that can be measured throughout a course of treatment through MR or ultra-CT imaging to allow patient-specific dosage and scheduling."
More information: Role of vascular normalization in benefit from metronomic chemotherapy: Insights from a mathematical model, PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1700340114