Study identifies gene—and drug target—involved in inflammation after injury
During a stroke or organ transplant, patients can suffer an injury due to lack of blood supply to vital organs. The injury—known as ischemia reperfusion—can cause damage to tissues. But a new Yale-led study has identified a previously unknown mechanism leading to the injury, and a potential target for drug treatment.
For the study, published in Cell Reports, the research team focused on a type of white blood cell called neutrophils. These cells mobilize to the site of an injury and protect the body from infection. But they also trigger inflammation that can damage tissues.
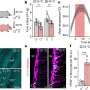
The researchers studied mice engineered to lack the function of a specific gene, PKN1, that had not yet been studied in immune cells. They learned that the PKN1 protein encoded by this gene can control the recruitment of the tissue-damaging neutrophils by regulating protein "traffic" inside neutrophils.
By describing the PKN1 pathway and its role in inflammation, the researchers have pinpointed a target for preventing injury. "The signaling pathway we identified provides a potential protein target to limit tissue damage during strokes and tissue transplantation," said corresponding author Wenwen Tang, associate research scientist in pharmacology. Other authors are Qianying Yuan, Chunguang Ren, Wenwen Xu, Jiasheng Zhang, Yong Zhang, and Dianqing Wu of Yale School of Medicine; and Björn Petri, and Paul Kubes of University of Calgary.
More information: PKN1 Directs Polarized RAB21 Vesicle Trafficking via RPH3A and Is Important for Neutrophil Adhesion and Ischemia-Reperfusion Injury. Cell Reports (2017). DOI: dx.doi.org/10.1016/j.celrep.2017.05.080 , www.cell.com/cell-reports/full … 2211-1247(17)30754-4