Holographic images increase accuracy of external ventricular drain insertion
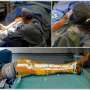
Researchers from Beijing have developed a new technique of external ventricular drain (EVD) insertion that involves the use of a mixed-reality holographic computer headset. Wearing this headset, the neurosurgeon can visualize holographic images of individual patients' brain structures while performing the procedure. This makes EVD insertion more accurate than the usual freehand technique, which relies only on referral to external anatomical landmarks. The new technique is described and illustrated in the article, "A wearable mixed-reality holographic computer for guiding external ventricular drain insertion at the bedside," by Ye Li, M.D., Ph.D., and colleagues, published today in the Journal of Neurosurgery.
External ventricular drainage systems are widely used to manage intracranial hypertension, intraventricular hemorrhage, and acute hydrocephalus. A catheter (drain) is inserted through the patient's skull and moved through brain tissue until it reaches a site within a ventricle (the target). Once there, intracranial pressure can be monitored, and blood or excessive amounts of cerebrospinal fluid can be removed via the drain.
Often conducted at the bedside of the patient, the neurosurgeon commonly performs EVD insertion using a "blind," freehand technique, in which he or she does not see the operative field. The neurosurgeon relies visually on anatomical landmarks on the outside of the patient's head and knowledge of normal brain anatomy underlying those landmarks. When performed in this manner, the procedure is only accurate about half the time and may require two or more passes of the catheter to reach the correct position in the ventricle.
If the brain is injured or diseased, brain structures may have shifted from their normal anatomical positions, making it more difficult to estimate the best pathway to the ventricle. Repeated passes of the catheter pose an increased risk of complications (hemorrhage or infection) to the brain.
Accuracy of the procedure can be increased by the addition of imaging guidance, but navigational devices are usually bulky and expensive, and add time to the procedure. They also necessitate transfer of the patient to the operating room. For these reasons, many physicians prefer not to use them.
Present Study
Li and colleagues set out to develop a new technique of EVD insertion that can easily be performed at the bedside and can provide greater accuracy than the blind, freehand technique. The one they have developed is guided by holographic images of individual patients' unique brain anatomy.
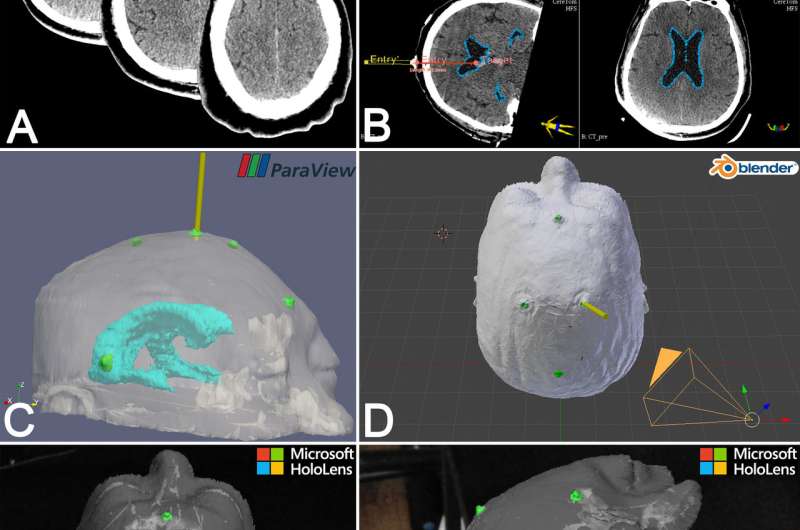
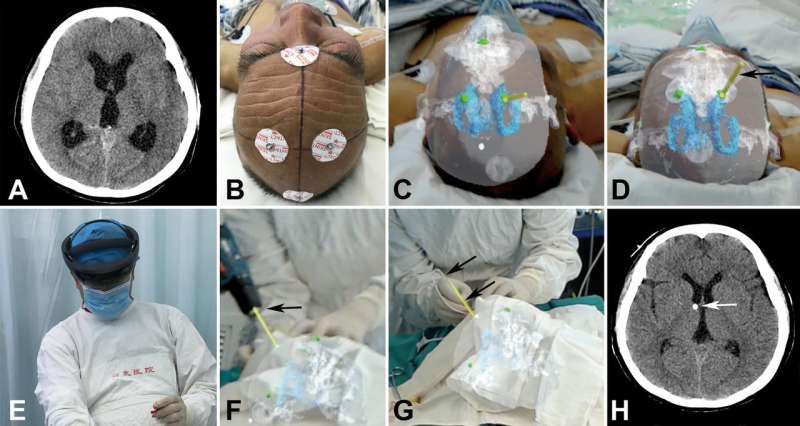
The researchers tested the readily available Microsoft HoloLens mixed-reality holographic computer headset while treating 15 patients. Registration markers, which can be identified on imaging studies, were attached to the head of each patient, and computed tomography (CT) was performed. Two-dimensional CT-generated data were converted into three-dimensional data, on the basis of which a surgical plan could be created. Then all this information was accessed by the wireless HoloLens headset and visualized by the neurosurgeon as holographic images. The holographic images resembled specific brain structures inside the head of the particular patient whose CT scans were used and included the planned trajectory of the catheter to the targeted site in the ventricle.
While wearing the HoloLens headset, the neurosurgeon was able to superimpose holographic images over the actual head of each patient and align the registration markers seen on the holograms with those attached to the outside of the patient's head. This allowed the neurosurgeon to "see" from outside the head into the brain of the individual patient, and to follow the course of the catheter as it moved along the planned trajectory to the ventricle. It also allowed for easy adjustments to the trajectory during the procedure, if necessary. An added benefit to the neurosurgeon was that "the mixed-reality device succeeded in creating the feeling of the actual physical presence" of brain structures within the patient's skull, making the entire surgical procedure more intuitive and natural.
No adverse events occurred in patients when holographic guidance was used. The mean number of passes required to reach the target in the 15 patients treated with holographic guidance was 1.07 ± 0.258 compared to 2.33 ± 0.98 in a control group of 15 patients in whom EVD insertion was performed using the blind, freehand technique. The mean target deviation was 4.34 ± 1.63 mm compared with 11.26 ± 4.83 mm in the control group. The differences in values between the two patient groups are statistically significant, thus showing significantly greater accuracy when the HoloLens headset was used.
Use of the holographic guidance system added a mean additional time of 40.20 ± 10.74 minutes prior to the procedure. This is not unlike the amount of additional time required when imaging-guided navigation is used. The authors believe that as they become more accustomed to working with the HoloLens headset, this preprocedural time will shorten. Despite the increased time, the procedure still can be used at the bedside and does not require bulky and expensive equipment.
The work reported in this paper is still preliminary. The authors acknowledge limitations of their study, including the small number of patients in the study group. However, they look forward to improvements in registration accuracy and simplicity of the procedure in the hope of using this technique for other types of surgical procedures in the future.
When asked about the study, Dr. Wang said, "To the best of our knowledge, this is the first positive experience with the use of such a new state-of-art technique to assist neurosurgeons in bedside EVD insertion. With further improvement in accuracy and simplicity, this wearable mixed-reality holographic computer could also serve as a portable and low-cost navigational device for multiple neurosurgical fields in the future. In addition to the function of navigation, the application of this technique would change the neurosurgical way of 'seeing is believing,' making the important structures visible around the lesion. Therefore, this will make surgery more minimally invasive and safe."
More information: Journal of Neurosurgery (2018). thejns.org/doi/full/10.3171/2018.4.JNS18124