Study shows the brains of people with schizophrenia-related disorders aren't all the same
A new multi-site brain imaging study in The American Journal of Psychiatry shows that sub-groups of people use their brains differently when imitating emotional faces—a task that reflects their ability to interact socially. Interestingly, individuals with schizophrenia do not have categorically different social brain function than those without mental illness, but fall into different sub-groups that may respond to different types of treatments. These findings call into question the most common research approaches in mental health.
"We know that, on average, people with schizophrenia have more social impairment than people in the general population," says senior author Dr. Aristotle Voineskos in the Campbell Family Mental Health Research Institute at the Centre for Addiction and Mental Health (CAMH) in Toronto. "But we needed to take an agnostic approach and let the data tell us what the brain-behavioural profiles of our study participants looked like. It turned out that the relationship between brain function and social behaviour had nothing to do with conventional diagnostic categories in the DSM-5 (Diagnostic and Statistical Manual of Mental Disorders)."
Most brain research in the mental health field compares a disease group to a non-disease or "healthy" group to search for biomarkers, a biological measure of mental health symptoms. This search for biomarkers has been elusive. This multi-site research study—which included 179 participants recruited at CAMH in Toronto, Zucker Hillside Hospital in New York and the Maryland Psychiatric Research Center in Baltimore—calls that paradigm into question because people with the same mental illness may not show the same biological patterns.
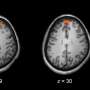
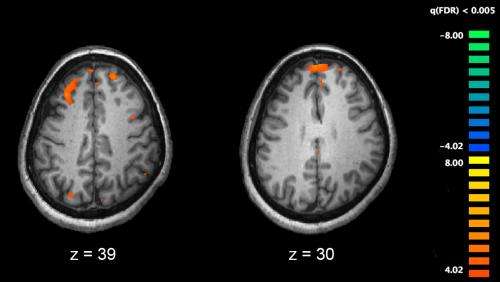
The study, which involved participants completing a facial imitation task while undergoing functional MRI brain scans, found three "activation profiles," says first author Dr. Colin Hawco, also of CAMH. These can be described as typical, over-activated and de-activated profiles.
"We think those with over-activated networks may be 'inefficient' in terms of brain activity—they probably struggled more and needed to work harder to do the same task compared to the other groups," says Dr. Hawco. "The 'de-activating' group seemed to show very efficient use of their brain, and did better on behavioural tests of social processing as well." These findings were true for participants with and without schizophrenia.
"There is really no effective treatment to deal with these social impairments, which is why we're really invested in figuring out the brain networks of social behaviours as targets for treatment and research," says Dr. Anil Malhotra, Director of Research at the Zucker Hillside Hospital. "We are now positioned to test treatments to help change brain function, rather than focusing on symptoms alone, when it comes to helping people with social impairment."
People with social impairments may not be able to react as expected to emotions they see in others, such as fear, sadness or happiness. "As social impairments become more severe, people are more likely to be isolated, unable to function in daily life, and have a marked reduction in their quality of life," says Dr. Robert Buchanan, Director of the Maryland Psychiatric Research Center, a psychiatrist and researcher who has been working to find new treatments to improve social function over the past three decades.
The findings were bolstered by an independent replication sample of 108 participants, which showed the same brain function findings as in the original sample.
More information: Colin Hawco et al, Separable and Replicable Neural Strategies During Social Brain Function in People With and Without Severe Mental Illness, American Journal of Psychiatry (2019). DOI: 10.1176/appi.ajp.2018.17091020